Introduction
Obstructive sleep apnea (OSA) is diagnosed when the airflow is disrupted due to the obstruction of one or multiple sites in the upper airway during sleep.1,2) The primary treatment for OSA is continuous positive airway pressure (CPAP), and alternative treatment choices such as oral appliances and surgical interventions are considered for patients who fail CPAP therapy.2,3) Drug-induced sleep endoscopy (DISE) is widely used to identify the site of obstruction before surgical treatment, with the oropharynx being recognized as one of the major sites contributing to airway closure.4) The harmonic scalpel, which operates at a vibration frequency of 55,500 Hz, is a surgical instrument that disrupts hydrogen bonds and induces protein denaturation.5) Although caution is required during its use due to the possibility for thermal damage to the surrounding tissues, there have yet been no published reports on burns caused by the harmonic scalpel during sleep apnea surgery. Herein, we describe a case study of a 49-year-old patient undergoing partial epiglottectomy for OSA, who experienced a burn injury to the right commissure of the mouth during the surgery performed using a harmonic scalpel.
Case Report
A 49-year-old woman with a 10-year history of persistent sleep apnea and no significant medical history other than diabetes complained of snoring and bilateral nasal congestion. Nasopharyngoscopy revealed hypertrophy of the inferior turbinate, deviated nasal septum, and enlarged tonsils. She was diagnosed with severe OSA (apnea-hypopnea index: 35.2) based on a polysomnography and initially treated with CPAP. However, due to discomfort, she discontinued CPAP and opted for surgical intervention. We performed DISE to identify the sites of airway obstruction, which revealed closure in the velum, base of the tongue, and epiglottis during sleep.
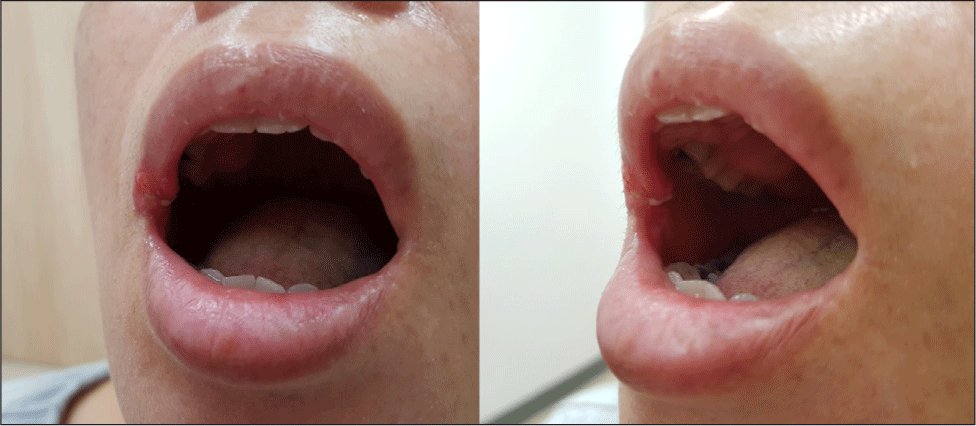
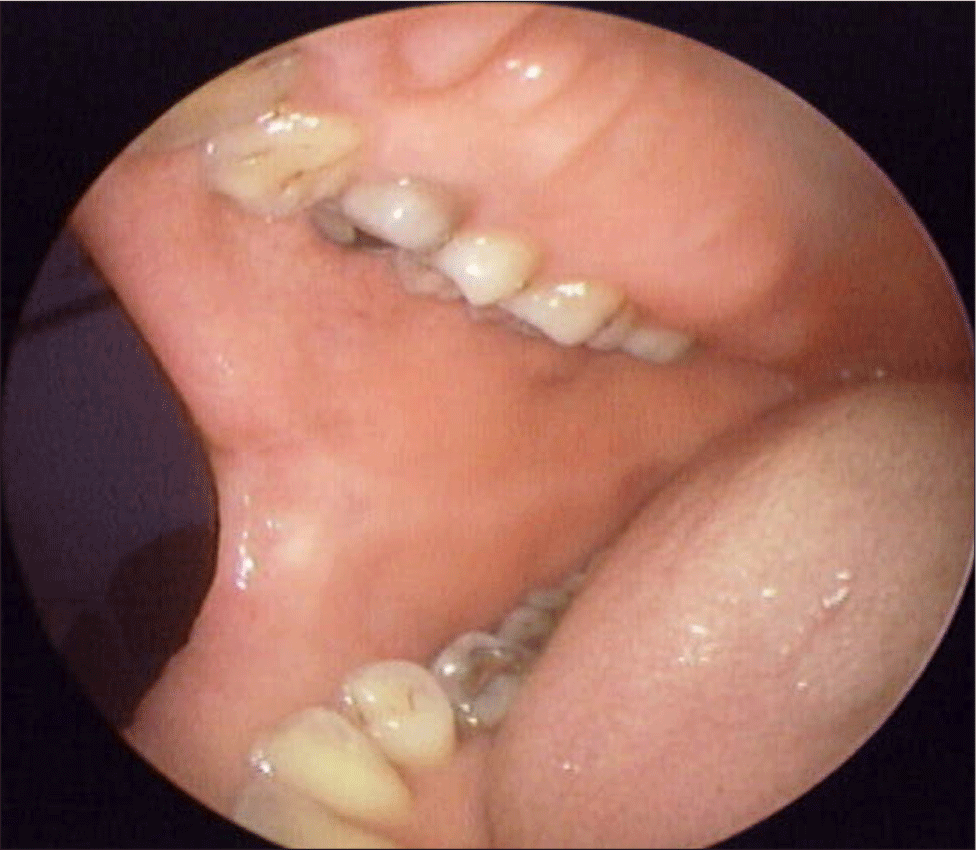
We first performed septoplasty and inferior turbinate reduction under general anesthesia. Subsequently, we conducted relocation pharyngoplasty and tonsillectomy using monopolar electrocautery device in the supine position, followed by exposure of the epiglottis using a suspended laryngoscope. When placing the suspended laryngoscope, attention was paid to damage to the teeth and lips, so the lips were observed, but no burn damage was found until then. The epiglottis was clamped with forceps, and approximately 40% of the upper portion of the epiglottis was excised using a Harmonic Ace Plus 7 (Ethicon, Cincinnati, OH, USA) scalpel set at level 5 power. Care was taken to ensure that the heat generated by the harmonic scalpel did not affect the surrounding tissues, and the partial epiglottectomy was completed. However, during recovery from anesthesia, we observed a second-degree burn on the patient’s right commissure of the mouth. After a dermatology consultation, wound care, including dressing and application of a steroid ointment, was initiated. At the 1-week postoperative follow-up, the burn injury on the right commissure presented signs of improvement but still exhibited erythema, edema, and blistering (Fig. 1). At 1 month after burn treatment, the lesion had healed without scarring or complication (Fig. 2). Both snoring and sleep apnea symptoms improved, and in polysomnography performed 6 months after surgery, apnea-hypopnea index decreased from 35.2 to 3.9 and nadir of oxygen saturation increased from 76% to 89%.
Discussion
OSA is a highly prevalent disorder in adults and commonly associated with reduced quality of life, increased risk of developing systemic diseases, and mortality rates.1,3,6) Among patients with OSA, the incidence of epiglottic obstruction ranges from 15% to a maximum of 70%, with cohort studies reporting a prevalence of 20%.4) Epiglottic obstruction during sleep can impede the airflow generated by CPAP, contributing to CPAP treatment failure.2,7) Therefore, additional interventions may be required for patients with OSA with epiglottic obstruction, which include the use of a mandibular advancement device, hyoid suspension, and uvulopalatopharyngoplasty.4)
The harmonic scalpel consists of a sharp cutting blade and a blunt protective blade.5,8) The cutting blade vibrates at 55,500 Hz, allowing effective sealing and cutting of veins and arteries up to 9 mm and also enables tissue cutting and coagulation to occur simultaneously.5,8,9) It is commonly used in head and neck surgery, gynecology, general surgery, and recently in laparoscopic procedures and endoscopic surgeries.8) Compared with high-frequency electrical currents or lasers, the harmonic scalpel requires less energy for tissue cutting and maintains relatively low temperatures (50℃–100℃) during use, causing minimal damage to the surrounding tissues.8) Furthermore, it generates less smoke and toxic byproducts from the thermal decomposition of fat and protein compared with that generated by other surgical instruments, contributing to improved surgical visibility.8) Emam et al. conducted an experiment on pigs and reported that when the harmonic scalpel was operated at level 5 power for 15 s, temperatures >140℃ were detected at a distance of 1.0 cm from the cutting site, but no tissue damage occurred when it was operated at level 3 power for <5 s.10) Similarly, Pogorelić et al. observed that with increases in the power level and usage time of the harmonic scalpel, the extent of thermal damage to the surrounding tissues and the depth of tissue injury also increased.8) Moreover, even with the same 10-s usage time, if there was an approximately 5-s interval of nonuse, the damage to the surrounding tissues was significantly reduced.8) In the present case, although the excision of the normal epiglottis did not need a significant amount of time, it is believed that the activation of the harmonic scalpel without special attention to the operating time and the consecutive activation without considering the contact of the instrument with the commissure during its removal resulted in thermal injury and subsequent burn damage to the right commissure of the mouth.
A first-degree burn occurring due to the use of the harmonic scalpel can generally be effectively treated with dressing and topical ointments, leading to minimal scarring and good recovery.11) However, a third-degree burn may leave permanent scars, requiring additional treatments such as steroid injections and tissue reconstruction surgery.11) It has been suggested that to prevent thermal damage to the surrounding tissues, especially when using instruments during transoral procedures, protective devices should be applied to the exposed areas of the skin. For instance, Nuara et al. used disposable cheek retractors on both sides of the cheeks to prevent burns around the mouth during tonsillectomy and adenoidectomy procedures.11) In our hospital, we take preventive measures by placing moist gauze over the exposed skin to minimize tissue damage.
Oral burns caused by electrocautery have been reported, but burns caused by harmonic scalpel have not been reported, and the risks caused by this are not well known because it is not a tool frequently used by rhinologists. However, use of harmonic scalpel has been increased recently to reduce bleeding when operating nasal tumors, so rhinologists also need to be aware of the possibility of these complications and be careful to use the instruments. In particular, surgeons pay a lot of attention to damage caused by electric devices to the surgical area, but we need to be careful when removing the tools out of the body, such as the mouth. If the electronic device is operated for a long time, the blade temperature rises, so if it is operated for a long time, it is recommended to use the tool while allowing the device to cool down for a while. Detailed explanations, both verbally and in written form, must be provided to patients and their guardian before surgery, including the risks associated with the use of surgical instruments and the importance of preventing burns to the surrounding tissues. This information should be included in the surgical consent form to ensure clear and comprehensive communication.






