Introduction
Tuberculous otitis media (TBOM) is a rare form of tuberculosis (TB) that accounts for approximately 0.05% to 0.9% of all chronic suppurative otitis media.1) It primarily occurs secondary to TB of the lungs, pharynx, larynx, and nose.2) It is hypothesized that TBOM can be caused by the inoculation of sputum or secretions contaminated with TB bacteria through the eustachian tube, rarely through hematogenous or lymphatic infection, or even direct infection through the tympanic membrane.1,2) There have been two reported cases of TBOM following nasopharyngeal tuberculosis (NPTB), both demonstrating unilateral TBOM, with the speculated cause being infection via the transfer of secretions from nasopharyngeal lesions.3,4) However, to date, there have been no reports of bilateral TBOM following NPTB. The current report presents a case that progressed to bilateral TBOM approximately one month after the onset of NPTB along with a review of the literature.
Case Report
A 42-year-old woman with no underlying condition presented with bilateral aural fullness. She had visited another hospital a month ago because of postnasal drip symptoms, where inflammatory lesions in the nasopharynx were discovered during nasopharyngoscopy. She was prescribed antibiotics and recommended nasal irrigation, but did not receive proper instructions on the correct irrigation method. Consequently, the continued use of improper techniques, such as swallowing during irrigation and tilting her head too laterally, reportedly caused aural fullness with each irrigation. Improvements in the nasopharyngeal lesions were not observed one week after nasal irrigation, and the patient developed additional aural fullness in the left ear. Paranasal sinus computed tomography (CT) revealed soft tissue density in the left middle ear, indicative of serous otitis media (Fig. 1A). Despite an additional month of antibiotic treatment, nasal irrigation, and one instance of myringotomy of the right tympanic membrane, no improvement was observed. Consequently, the patient was referred to our hospital.
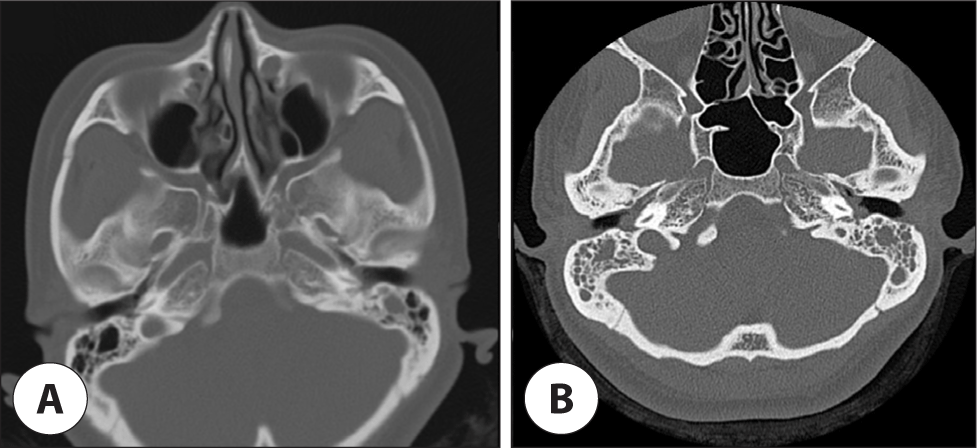
Otoscopy revealed a small perforation of the tympanic membrane and bilateral serous otorrhea (Fig. 2A, B). After suction of the otorrhea, a whitish mass was observed through the perforated area of the left tympanic membrane, which was presumed to be granulation tissue in the middle ear. Standard pure-tone audiometry revealed conductive hearing loss, with air conduction at 38 dB and bone conduction at 17 dB on the right and air conduction at 40 dB and bone conduction at 8 dB on the left. During nasopharyngoscopy, a crust formation was observed in the nasopharynx, prompting a tissue biopsy (Fig. 2C). Biopsy results showed necrotic granulation tissue positive for acid-fast bacilli culture. Polymerase chain reaction (PCR) for the Mycobacterium tuberculosis complex (MTB) and nontuberculous mycobacteria yielded positive MTB results. A temporal bone CT scan conducted on the day of the first outpatient department visit (approximately one month after symptom onset) showed soft tissue density filling both the middle ear and mastoid cavities, without bone destruction (Fig. 1B).
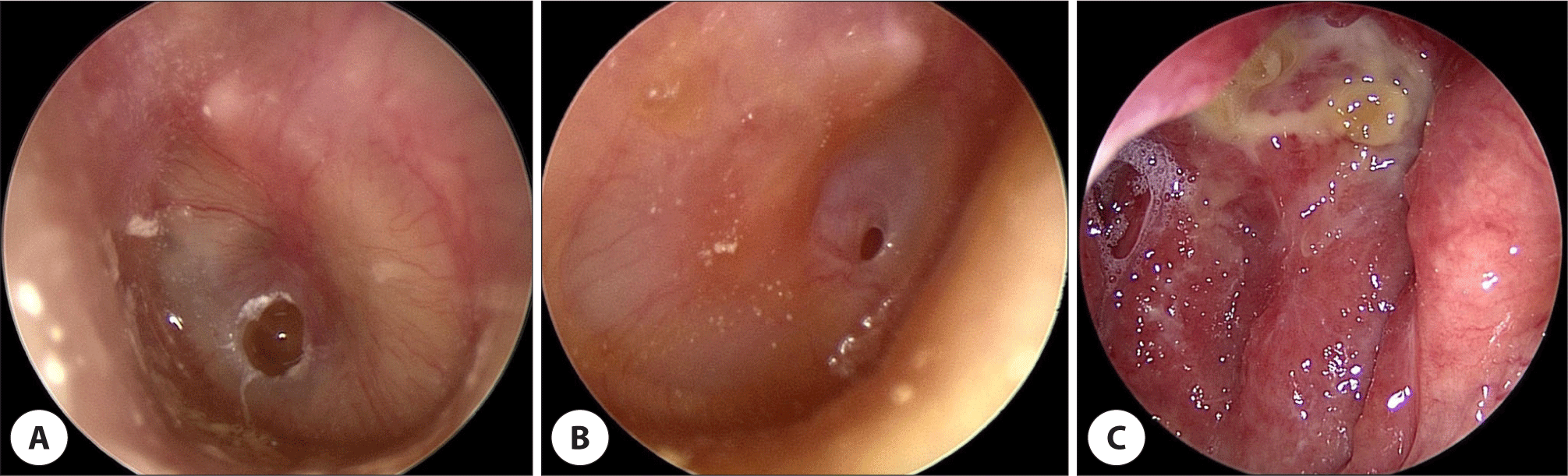
Further PCR tests for otorrhea confirmed bilateral TBOM. Chest CT performed upon referral to the Department of Infectious Diseases and Respiratory Medicine revealed no abnormalities. The patient fully recovered after nine months of treatment with isoniazid, ethambutol, rifampin, and pyrazinamide. Currently, 14 months after the onset of symptoms, the patient’s hearing and perforation of the tympanic membrane have improved. There are no signs of recurrence in the nasopharynx or middle ear, and no haziness was observed in the mastoid cavity on CT (Fig. 3).
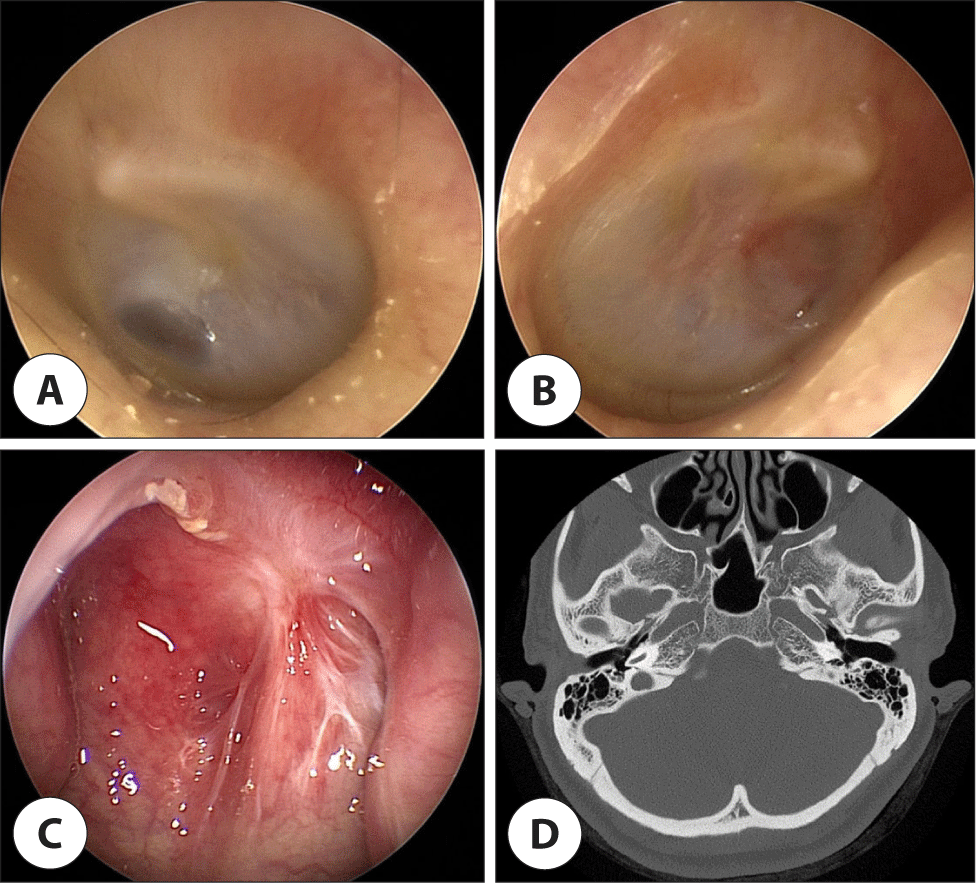
Discussion
NPTB, either primary or secondary to lung TB, is usually caused by direct inhalation of airborne TB bacteria or exposure to TB-laden sputum.3) Similarly, TBOM can be transmitted from sputum via the eustachian tube or from systemic TB lesions through hematogenous or lymphatic spread.1,2)
Clinical manifestations of NPTB include rhinorrhea, postnasal drip, nasal obstruction, epistaxis, ulcerative lesions, masses, and crust formation.5) TBOM initially presents with nonspecific symptoms such as painless otorrhea, aural fullness, and multiple tympanic membrane perforations. These nonspecific features often lead to delayed diagnosis, and bone destruction is observed in later stages.6)
In cases in which the nasopharynx is the primary site of TB with no respiratory symptoms, it is necessary to consider the differential diagnoses that present similar local findings. These typically include nasopharyngeal cancer, sarcoidosis, fungal infections, autoimmune diseases (Wegener’s granulomatosis, polyarteritis nodosa, and Churg-Strauss syndrome), and granulomatous inflammation (sarcoidosis, syphilis, leprosy, and midline lethal granuloma). Although tissue biopsy is essential for differential diagnosis, confirmation cannot rely solely on pathological findings, as caseous necrosis may not always be identifiable.7)
Following the collection of specimens, either tissue or discharge, PCR is the most reliable method to confirm NPTB and TBOM.1,3,5,6) However, cases have been diagnosed based on positive results from the QuantiFERON TB blood test or the TB-specific interferon-gamma test, despite negative TB-PCR results. Therefore, additional tests should be considered if TB-PCR results are negative.3)
In this case, the patient developed bilateral TBOM within one month of NPTB discovery. To date, two cases of concurrent NPTB and TBOM have been reported; however, both were unilateral and there are no reports of bilateral TBOM after NPTB. The significance of this case lies in investigating why TB bacteria spread to both middle ears within one month after NPTB diagnosis, rather than the mere fact that it resulted in bilateral TBOM.
We speculate that improper nasal saline irrigation significantly contributed to the rapid spread of TB to both middle ears. The patient reported frequent swallowing of saline while excessively tilting her head and positioning the contralateral eustachian tube towards the floor during irrigation. Nasal saline irrigation is generally known to be safe without serious adverse effects. However, there is no scientific consensus regarding the optimal quantity, frequency, or methods of nasal irrigation. Caution should be exercised when using contaminated saline.8) Patients should avoid tilting their heads too far to the side because of the anatomical position of the eustachian tube, for the following reasons. The eustachian tubes open for approximately 200–400 ms during swallowing.9) Typically, owing to the anatomical structure, the eustachian tubes drain from the middle ear towards the nasopharynx at a downward diagonal angle.9) However, when the head is tilted excessively to one side, the middle ear is positioned lower than the nasopharyngeal opening of the eustachian tube, enabling the irrigation fluid to flow back into the middle ear. This can result in aural fullness, a known adverse effect of nasal irrigation.8)
Additionally, a CT scan performed at another hospital during the first week of nasal irrigation showed no particular findings except for some soft tissue density in the left mastoid cavity. However, the CT scan conducted at our hospital one month after nasal irrigation showed that both mastoid cavities were completely filled with soft tissue density. Given these circumstances, it seems plausible that improper nasal irrigation led to the rapid spread of NPTB in both middle ears.
Conclusion
The present case report highlights the role of tissue biopsy and TB-PCR in the early diagnosis of TB when nasopharyngeal lesions or otitis media do not respond to typical antibiotics and symptomatic treatments. Even before the diagnosis of NPTB is made, it is essential to educate patients on the correct nasal irrigation method. In particular, if NPTB is diagnosed, avoiding nasal irrigation may reduce the risk of NPTB spreading to the middle ear.






