Introduction
Necrotizing sialometaplasia (NSM) is a rare, benign, and self-limiting disease of salivary glands. It classically involves mucoserous glands of hard plate adjacent to the soft palate. It presents as a single and unilateral ulcer. Although the etiology of NSM has not been clearly determined, events that can cause ischemic injury of mucoserous glands (such as dental injection, blunt trauma, denture wear, alcohol, smoking, or upper respiratory infection, etc.) are known to precede the occurrence of NSM.1,2) The clinical feature of NSM alone makes it difficult to distinguish it from minor salivary gland tumors including malignant tumor because it is observed as a single and large ulcer that commonly persists more than a month.3) Therefore, appropriate biopsy for ulcerative lesion is crucial for diagnosing NSM. In addition, the physician should discriminate NSM against malignant tumors until completion of wound healing and providing counseling about the healing course of NSM to the patient is necessary. We now report our experience in diagnosing and treating NSM with a detailed review of histologic results.
Case Report
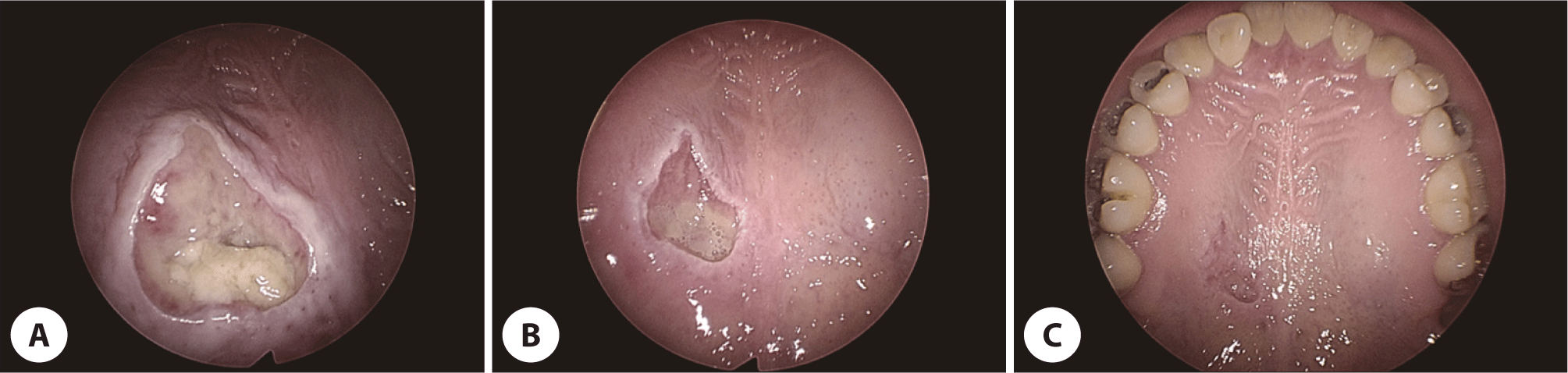
A 27-year-old female without past medical history or underlying disease was referred to our clinic because of pain and swelling of right-side hard palate that persisted and aggravated for two weeks despite non-steroidal anti-inflammatory drug medication. The patient clearly stated that there was no possibility of ischemia history in the oral cavity. On physical examination, an ulcerative lesion about 2 cm with central necrosis on hard palate adjacent to soft palate was observed (Fig. 1A). However, there was no other palpable lesions of the neck.
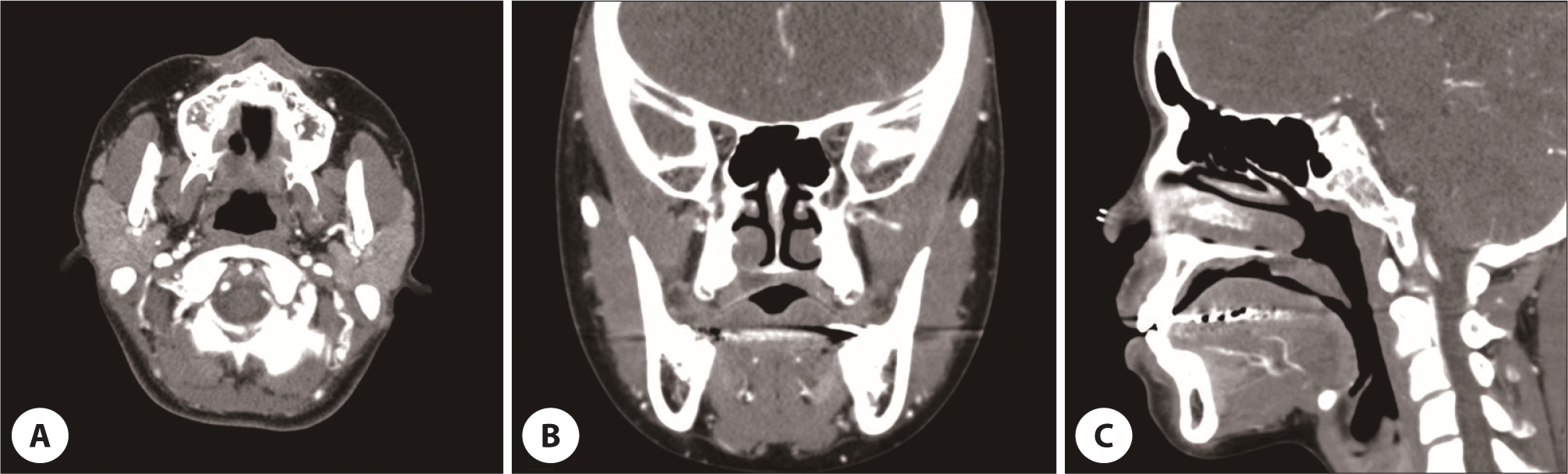
We suspected a tumor originating from a minor salivary gland and explained the possibility of a malignant tumor to the patient. Before performing an incisional biopsy for the ulcerative lesion, computed tomography (CT) was performed. An ulcerative lesion about 15×23 mm in size with peripheral enhancement on right hard palate was identified on CT scan (Fig. 2A). However, there were no bony erosions under the ulcerative lesion or significantly enlarged lymph nodes (Fig. 2B, C). Biopsy was performed at two areas. One was on the ulcer margin including a pinkish mucosa and the other was on the central necrotic part.
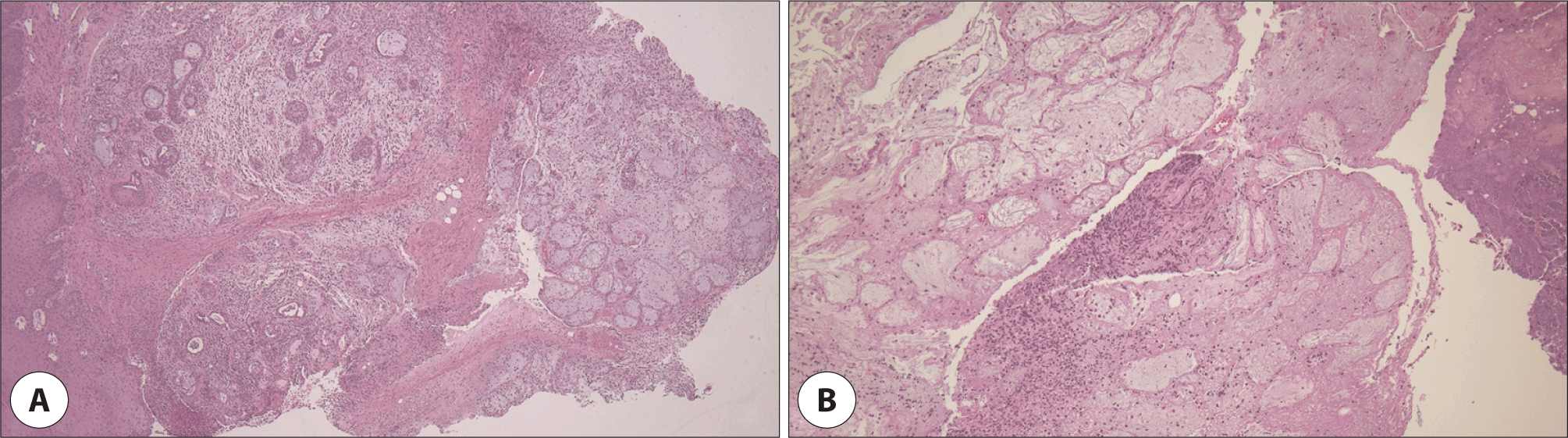
The specimen obtained from the ulcer margin showed mucin spillage, necrosis, and squamous metaplasia of acini and ducts (Fig. 3A). There was no destruction on salivary gland structures (Fig. 3A). On the central lesion, an intact lobular architecture of salivary gland was observed. The necrotic tissue mostly consisted of necro-inflammatory exudate with bacterial colonies (Fig. 3B). We finally diagnosed it as NSM based on results of histopathologic findings.
We prescribed short-term medication including cefditoren 100 mg three times a day and prednisolone 5 mg twice a day for 5 days after the biopsy. At one week after the biopsy, the biopsy site was on the healing course, showing a decrease in its size (Fig. 1B). As the patient’s subjective symptom of pain was much decreased, we prescribed benzydamine hydrochloride gargle 1.5 mg/mL at 15 mL a day for one week considering its anti-inflammatory, analgesic, and antipyretic effect.4) At three weeks after the biopsy, the biopsy site was nearly healed (Fig. 1C). Another two weeks after the last visit, the patient’s biopsy site was finally healed on a telephone survey, which was seven weeks after the onset.
Discussion
We successfully treated a young female patient with conservative management without surgical excision through detailed review of histology. NSM clinically has similar features of malignant neoplasm of minor salivary gland which commonly presents with ulceration and painless submucosal swelling fixed on overlying mucosa. Therefore, NSM can be easily misdiagnosed as a malignant tumor, leading to surgical excision sometimes. Understanding the clinical progress and biopsy results of NSM can prevent overtreatment.
NSM is generally known to be preceded by any type of traumatic events that can cause tissue ischemia. However, in our case, NSM was diagnosed without a definite trauma history. NSM is predominant in males than in females.1,5) It clinically arises in hard palate unilaterally. There is no sufficient clinical clue to exclude NSM from malignancies. In our case, the central part of the lesion was totally consisted of necrosis and the outer rim was slightly protruded on physical examination. Other study of hard palate malignancy, its clinical features were similar to our case, such as ulcerative lesion on the hard palate.6) As CT sometimes shows bony erosion near the ulcerative lesion or abnormal lymph nodes on malignancy, CT might be helpful in discriminating malignant tumor such as mucoepidermoid carcinoma or squamous cell carcinoma which has similar clinical features to NSM. Although it has a limitation because typical changes observed in CT might not be seen in early cancer, disease extent provided by imaging study help discriminate NSM with malignant tumor. There is a case that reported delayed diagnosis of malignant tumor previously diagnosed as NSM.7) Therefore, simultaneous imaging study may prevent delayed diagnosis of malignancy.
Detailed review of histologic finding enabled to diagnose NSM. Histologic features of NSM are squamous metaplasia of ducts and acini, lobular infarction with or without mucin spillage, inflammation, and necrosis while preserving lobular architecture of salivary glands.8) The perineural invasion, neoplastic goblet cells, or atypical mitoses should be carefully reviewed as those are typical features of malignancies.2) However, NSM has possibilities to be misdiagnosed as squamous cell carcinoma of salivary gland showing squamous metaplasia of salivary duct and high grade mucoepidermoid carcinoma of salivary gland showing necrosis.9,10) In addition, a case of NSM accompanied by adenoid cystic carcinoma has been described in previous study.10) We biopsied two sites for obtaining sufficient specimen. One included the ulcer margin and the other included the central necrotic part. The specimen from the ulcer margin clearly showed metaplasia with inflammatory background without destruction of salivary gland architecture. On the other hand, necrosis was dominantly shown in the central lesion specimen. While tissue metaplasia accompanied by necrosis of surrounding structure is a crucial description for diagnosing NSM, specimen taken only from central lesion will provide limited information. Consequently, it is important to obtain sufficient specimen of ulcer margin.
NSM generally shows a long natural healing course of about 2 to 3 months. In our case, it took a total of 7 weeks from onset to complete healing and patients with NSM eventually heal without any complications.2,3) Since delayed or incomplete healing of ulcerative lesion is a common clinical manifestation of malignancy in oral cavity, confirming the complete healing of ulcer is essential. Classically, NSM is known to be healed without any treatment. However, in our case, the patient’s subjective symptom of pain persisted two weeks and it was dramatically improved by prescribed antibiotics and short-term oral steroid after biopsy. Since inflammation accompanied by bacterial colony formation on specimen was observed on histologic examination, short-term oral antibiotics and steroid may accelerate the healing process of NSM.
In conclusion, NSM has a relatively long course to complete healing. It is difficult to distinguish NSM from malignancies before histological diagnosis. Even after biopsy, NSM might be mistakenly diagnosed as mucoepidermoid carcinoma or squamous cell carcinoma. A case of NSM accompanied by adenoid cystic carcinoma has been reported.11) Therefore, clinicians should obtain adequate specimen for histologic evaluation to prevent overtreatment of NSM, provide detailed clinical history to histopathologists for detailed review, and provide patient with information about a long process of healing of NSM. Lastly, observing complete healing of ulcerative lesion should be closely monitored in patients with NSM.






