Introduction
Since the term hemangioendothelioma (HE) was first used by Mallory1) in 1908, its definition has been changed over time by several authors. Recently, as proposed by Weiss and Enzinger2) in 1982, the definition of HE has been limited to vascular neoplasms showing a borderline biological behavior intermediate existing between entirely benign hemangiomas and highly malignant angiosarcomas. The category of this disease includes spindle cell HE, papillary angioendothelioma, epithelioid HE, kaposiform HE, pseudomyogenic HE, composite HE (CHE), and retiform HE (RHE). Definitive diagnosis among the various types of this disease is based on histopathological morphology and immunohistochemical markers.3) RHE was described by Calonje et al.4) in 1994, where it was to be considered a type of HE with a low rate of metastasis and a high rate of local recurrence. It is known to occur mainly in the upper and lower extremities, the trunk, and the head and neck area, but it is never reported in the paranasal sinus. To our knowledge, this is the first study to report the observation of RHE in the nasal cavity.
Case Report
A 53-year-old woman visited the ophthalmology outpatient clinic with a problem of a palpable lump on the medial side of the left lower eyelid for several years. The mass was painless and exhibited no change in size, so it has been observed without treatment. Symptoms of olfactory dysfunction appeared 3 months earlier. She experienced complete loss of left visual acuity due to trauma 30 years ago. On ophthalmologic examination, the left eyeball was displaced in the superolateral direction, and its movement was impaired; however, she was not aware of the time of onset. She had no past history except hypertension.
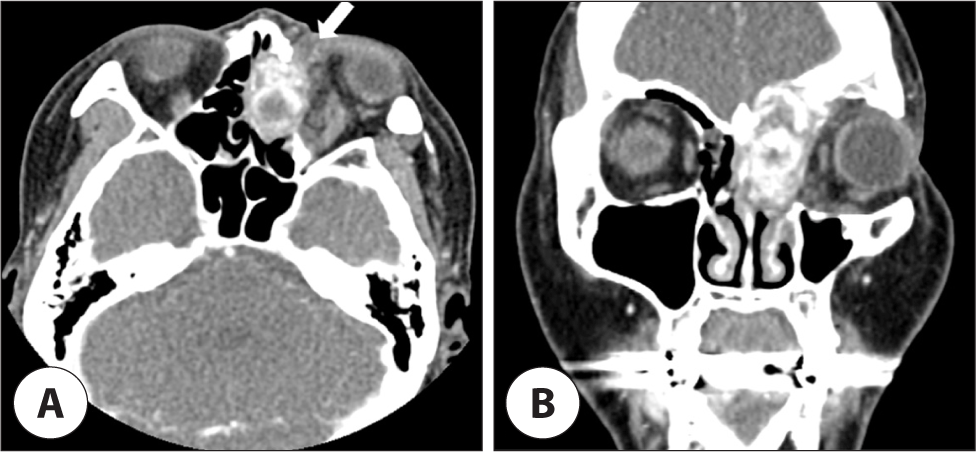
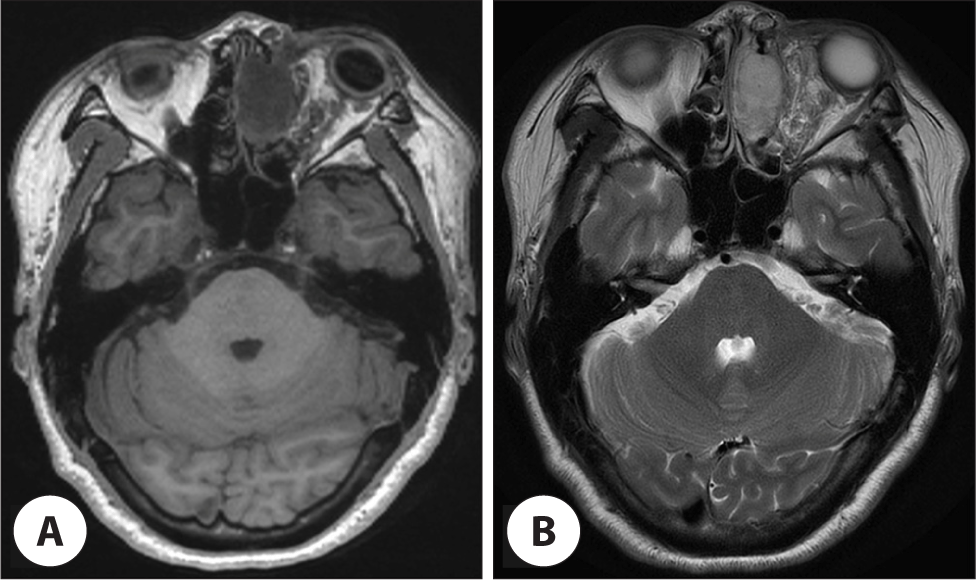
On contrast-enhanced computed tomography (CT), an expansile heterogenously intensely enhancing mass was observed in the left frontoethmoid sinus, which was accompanied by bony erosion of the orbital wall, and intracranial extension was suspected. Moreover, an ill-defined infiltrative soft tissue lesion in the extraconal and intraconal spaces of the left orbit was shown to extend to the periorbital area, which was considered to be a type of venolymphatic malformation (Fig. 1). Orbit magnetic resonance imaging (MRI) showed that the lesion located in the ethmoid sinus had low T1 and high T2 signals with good gadolinium enhancement, containing hemorrhage component and curvilinear T1/T2 dark signal (Fig. 2).
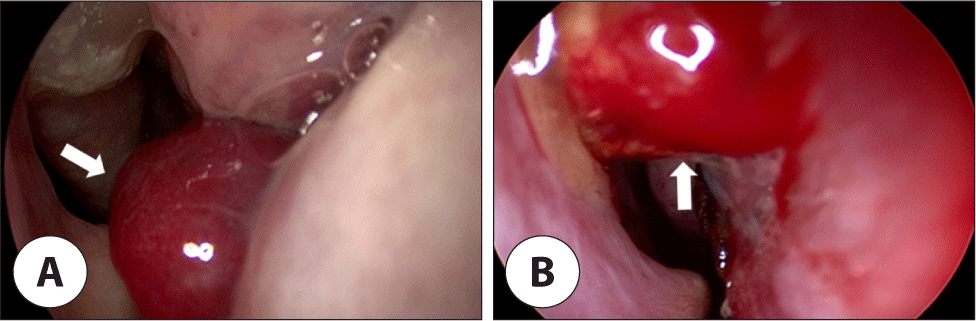
A biopsy was performed under local anesthesia for neoplastic lesions observed in the left conjunctiva by ophthalmology. On pathologic examination, multiple dilated lymphatic channels of variable sizes with lymphocytic infiltration were observed, which was suggestive of lymphangiectasia. The mass located on the lower eyelid was judged to be the same as the tumor in the sinus cavity, so the patient was referred to the otorhinolaryngology for evaluation and treatment of the sinus tumor. A hemorrhagic polyp was found in front of the uncinate process on the nasal endoscopy (Fig. 3A). An endoscopic biopsy was performed under local anesthesia at an outpatient clinic. Hemangioma was suspected in the form of closely packed vascular structures without any malignant features in the pathologic report.
For the lesion, which was confirmed as intraorbital lymphangiectasia, it was decided not to perform surgical resection due to the burden of orbital extraction. On the other hand, left endoscopic sinus surgery was planned under general anesthesia to remove the tumor located in the nasal cavity and sinuses. Vascular embolization was performed in the distal part of the left internal maxillary artery the day before surgery due to the possibility of intraoperative massive hemorrhage. During surgery, a mass lesion extending from the anterior ethmoid sinuses to the periorbita, frontal sinus, and anterior skull base was observed. Further, the tumor was encapsulated and accompanied by organizing hematoma in appearance. The tumor was fragile, and it was removed in a piecemeal manner. The lamina papyracea and skull base bone were partially lost due to the pressure effect on the tumor. A frozen biopsy was conducted to obtain benign findings.
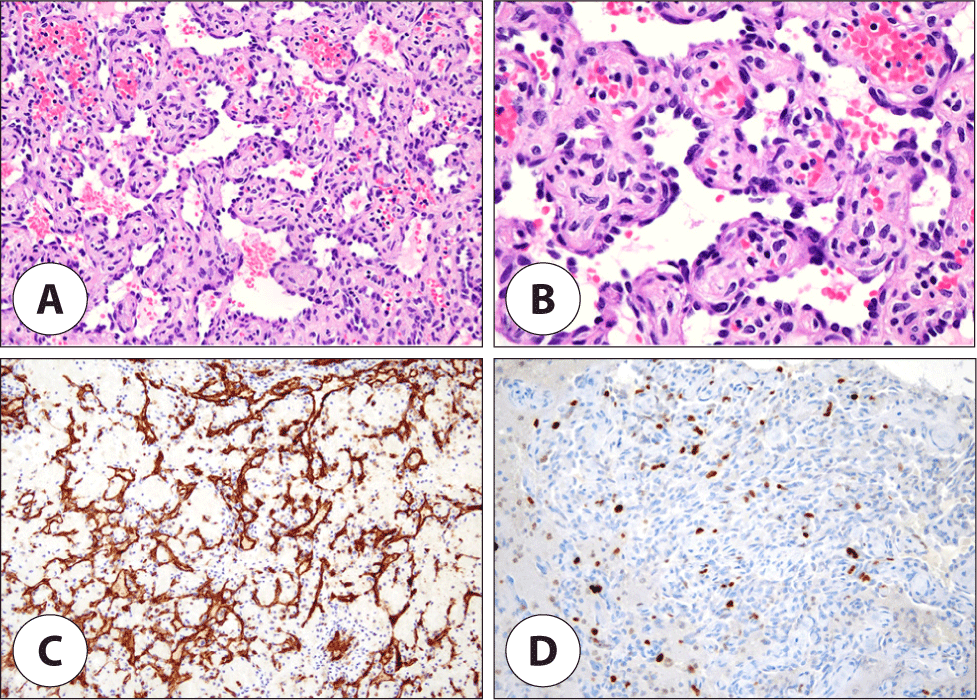
Postoperative histopathological examination revealed vascular proliferation composed of interconnecting arborizing blood vessels arranged in a retiform pattern, which were lined by monomorphic, hobnail endothelial cells. No significant cytologic atypia or mitotic figures were identified. The tumor demonstrated prominent hemorrhage with ectatic vessels and mild lymphocytic infiltrate in the stroma (Fig. 4A, B). Moreover, the immunohistochemical stain results were positive for CD31 and D2-40 in endothelial cells (Fig. 4C). Ki-67 showed a low proliferation index in tumor cells (11%) (Fig. 4D). The lesion was negative for both HHV8 and neuroendocrine marker (synaptophysin, CD56). Based on these features, it could clearly be diagnosed as RHE.
Recurrence of nasal endoscopy appeared 4 months after surgery (Fig. 3B), so a second operation for volume reduction was performed followed chemoradiotherapy with cisplatin. There was no evidence of recurrence for 7 months after this treatment.
Discussion
Most reported cases of RHE originate from cutaneous or superficial portions of the body, except for two cases of primary bone tumor reported by Aditya et al.5) and Kim et al.6) It occurred in the head and neck area in approximately 15% of cases, including scalp, canthus, pinna, parietal bones, and infratemporal fossa. To our knowledge, there have been no cases found in the nasal cavity.
Clinically, lesions of RHE appear as a solitary, slow-growing exo-endophytic mass, resulting in a characteristic of subcutaneous firm nodule.3) There has been a female predominance, but the remarkable predominant generation has yet to be defined.6)
The differential diagnosis of RHE includes Dabska’s tumor, malignant lymphoma, dermatofibrosarcoma protuberans, bacillary angiomatosis, Kaposi’s sarcoma, targetoid hemosiderotic hemangioma, and angiosarcoma.4,7) Histopathological examinations are needed to confirm the diagnosis of RHE it does not have unique clinical or radiological features. RHE consists of elongated arboreal vessels arranged in an anastomotic pattern in a manner similar to rete testis. Neoplastic vessels are lined with a single layer of hobnail-like endothelial cells protruding within the narrow lumina.3) Immunohistochemically, hobnail-like cells lining the elongated vascular space express endothelial markers, including von Willebrand factor, CD31, and CD34.8) Spindle cells in the solid region are positive for CD31 but negative for von Willebrand factor and CD34. Whether or not it responds to D2-40 remains controversial.9,10)
In our case, the area judged to be hemangioma was partially observed. It could be diagnosed as CHE because the tumor tissue had various vascular components. CHE—which is defined as a vascular neoplasm presenting combinations of benign, low-grade, and high-grade malignant components—was initially described by Nayler et al. in 2000.11) The most frequent histological component observed in CHE is retiform type, followed in order by epithelioid and spindle cell HE. Some benign components, such as cavernous hemangioma and arteriovenous malformations, may also be observed.12) However, the hemangioma-like area accounted for less than 10% of the total specimen in our case, so it is arguable whether it can be diagnosed as CHE. The definition of CHE still fails to provide both ‘minimal’ and ‘maximal’ criteria for diagnosis, and some published cases are better interpreted to be representing other tumors.13)
Although a definitive treatment option has yet to be established, surgical excision has been performed in most patients with RHE to this point. Hirsh et al.7) reported that chemoradiotherapy with low-dose cisplatin successfully treated RHE without surgical resection. Local recurrence is common; half of RHE has a mean recurrence period of about 12 months after surgery.6) However, metastasis is known to be rare. Even though RHE locally recurs with a high rate, no deaths have been reported. In our case, chemoradiotherapy was performed for local recurrent lesions after surgical attempt, and there has been no further evidence of recurrence to date. In the first operation of our case, endoscopic sinus surgery for biopsy was performed, and it is believed that a definitive treatment was not performed because the histological diagnosis was not certain. To reduce possible recurrence, there may be a need for an external approach with craniofacial resection.






