Introduction
Vocal fold paralysis (VFP) can occur due to various causes including viral infections, brain diseases, and surgical or traumatic injury to the laryngeal nerve. In these patients, the inability to fully close the glottis can result in breathy, unpredictable voices as well as dysphagia and decreased cough strength. Hoarseness related to a cardiovascular lesion is an unusual presentation. Ortner first described a case of left VFP due to compression of the recurrent laryngeal nerve (RLN) by a dilated left atrium with mitral valve stenosis.1) After that, various cardiovascular lesions associated with left RLN paralysis have been reported. This syndrome is currently called as cardiovocal syndrome.2–5) Mitral stenosis was the most common underlying illness in the previously described cases of Ortner’s syndrome.6–8) Other reports have suggested that left RLN paralysis can be accompanied by various clinical conditions including left ventricular failure, atrial septum failure, arterial canal persistency, primary pulmonary hypertension, relapsing embolism of the pulmonary artery, left ventricular aneurysm, and various types of aortic aneurysms.9–12) Here, we present three cases of Ortner’s syndrome occurring as a sac-like aneurysm of the aortic arch, combined with an intramural thrombus, intramural hematoma of the aortic arch, and a dissection-like giant aneurysm in the aortic arch directed inferiorly.
There are various options available to patients with unilateral VFP to improve their quality of life. In order to achieve optimal function, a team approach is required that provides the patients with both anatomic and technical tools to generate good voice. As the laryngologists focus on the treatment methods and procedures, the speech language pathologists concentrate on patient behavior and voice quality. The ideal surgical treatment would move the vocal fold margin medially so that the mobile vocal fold would meet it without interfering with phonatory vibration of either.13,14) Over many decades, the technique has been refined and it has emerged as an essential tool for surgical voice rehabilitation.
In 1974, Dr. Nobuhiko Isshiki of Kyoto University, Japan, described several types of laryngoplasty including the one that accomplished medialization of the vocal fold and improved glottic closure.15) Injection laryngoplasty is a treatment that has grown in popularity in recent years as a result of its low procedural cost, technical feasibility, and clinical success. It provides functional voice improvement in patients with unilateral VFP and it can also be utilized as a supplement to laryngeal framework surgery. It generally carries fewer risks compared to laryngeal framework surgery.13,16) However, there are several risks such as bleeding, infection, pain, and airway obstruction. Airway obstruction can occur secondary to over-medialization of the vocal fold and laryngeal edema, and it can rarely occur secondary to laryngeal spasm due to over-manipulation of the larynx. When bilateral injections are necessary, they should be performed with caution in particular for avoiding over-injection.17,18) Here, we discuss the management and the pathogenesis of unilateral VFP related to cardiovascular disorders with review of literature.
Case Reports
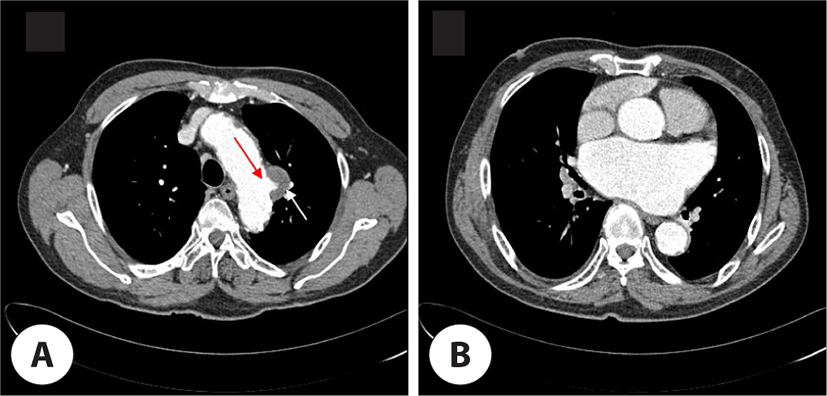
A 75-year-old male presented with hoarseness of voice and cough since 2 months. He was an ex-smoker with a 40 pack-year history. He had high blood pressure and a past history of percutaneous transluminal angioplasty because of total occlusion of the superficial femoral artery 4 years ago. Laryngoscopic examination revealed a paralyzed left vocal fold in paramedian position. Chest X-ray (posteroanterior view) showed cardiomegaly. In order to evaluate if there are any abnormalities in the lower neck area from the upper mediastinum area, where the RLN travels, we undertook contrast enhanced chest computed tomography (CT). Chest CT showed presence of a sac-like aneurysm of the aortic arch (2.6×1.9 cm) combined with an intramural thrombus (Fig. 1A). It was highly suggestive of Ortner’s syndrome due to aneurysm in the aortic arch. Further it showed a large heart size, especially left atrial enlargement (Fig. 1B). Electrocardiogram (ECG) showed atrial fibrillation without palpitation. Echocardiography showed severe degenerative atrial stenosis which was aggravated compared to that in a previous study. The patient underwent thoracic endovascular aneurysm repair (TEVAR) 1 year after the initial diagnosis at other tertiary hospital. He complained of breathy voice with aspiration. After adequate preparation, patients were positioned sitting upright in a chair or lying flat with neck slightly extended to allow access to the neck and larynx. A needle and a syringe containing the injection material were inserted in the cricothyroid notch and advanced through the cricothyroid membrane supero-laterally into the paraglottic area. 0.5 cc of low molecular hyaluronic acid was then injected until a desired position of the vocal fold was achieved and the patients were observed for 1 hour prior to discharge. Patients were informed that medialization thyroplasty may be necessary in case of permanent VFP in the future. His voice and aspiration were immediately improved and the improvement lasted for 4 months after the initial injection. We performed 3 more injections after the first injection every 4–6 months (Fig. 2A, D). For the perceptual analysis GRBAS scale was performed by a trained listener (speech language pathologist), of vocal quality on grade, roughness, breathiness, asthenia, and strain, all on a four-point scale (0–3) (sum range: 0–15). The initial GRBAS score was 8 and final GRBAS score was 3.
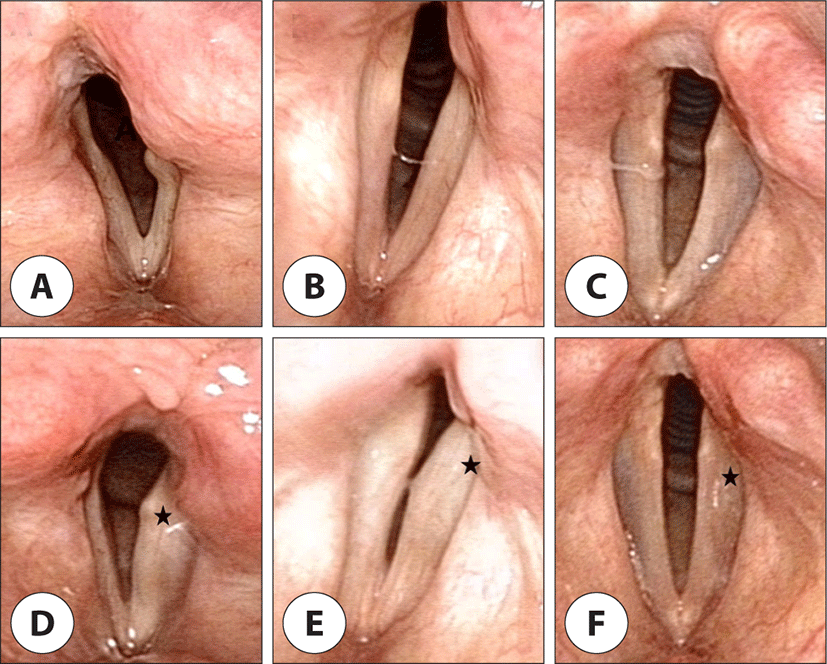
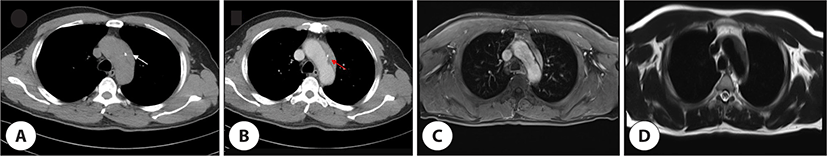
A 57-year-old male presented with hoarseness of voice since 1 month. He was a smoker for the last 40 years. He did not have any other symptoms such as cough, dyspnea, dysphagia, or weight loss. On examination, high blood pressure was noted. There was no cervical lymphadenopathy. Laryngoscopy revealed a paralyzed left vocal fold in paramedian position. Contrast enhanced chest CT image showed intramural hematoma of the aortic arch which displayed high attenuation in a non-contrast image that was highly suggestive of Ortner’s syndrome (Fig. 3A, B). ECG showed left atrial enlargement with left ventricular hypertrophy. Chest magnetic resonance imaging (MRI) was performed to evaluate the characteristic of intramural hematoma and showed a mass-like lesion of 1 cm thickness along the long axis of the aortic arch. This lesion showed intermediate and high signal intensity on T1- and T2-weighted images (Fig. 3C, D). We injected 0.5 cc of hyaluronic acid into the mid portion of the membranous vocal fold. His voice was immediately improved after the initial injection (Fig. 2B, E). We are currently following him up and we plan to perform repeat injection when his voice is aggravated. The initial GRBAS score was 6 and final GRBAS score was 2. Further 6 months follow up chest CT showed absence of hematoma spontaneously in this patient.
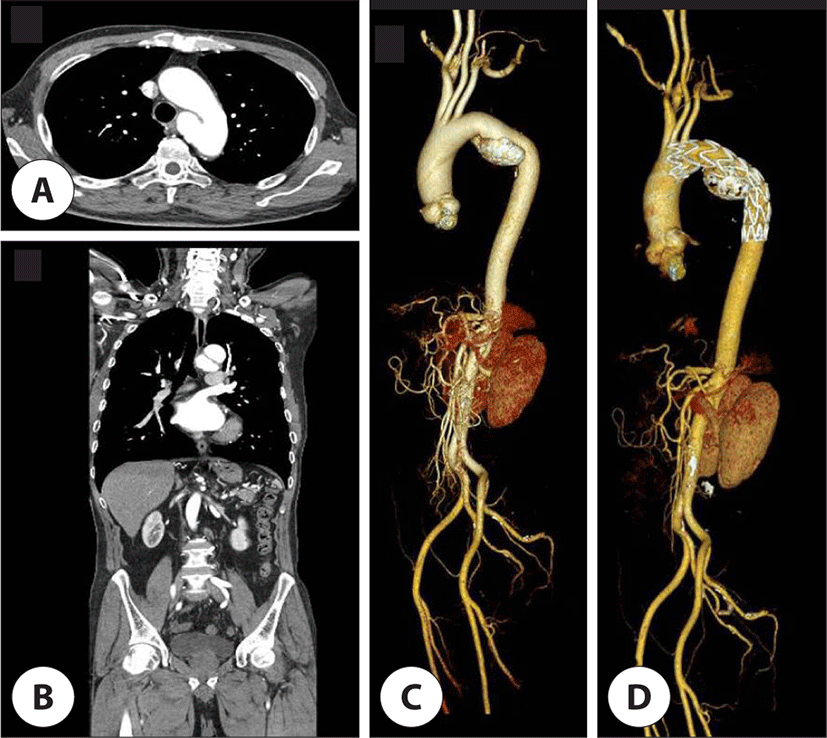
A 67-year-old male patient presented with hoarseness of voice of 1-year duration. He was an ex-smoker and he had been previously diagnosed with a left proximal descending aortic aneurysm and was followed up at our department of cardiovascular surgery. Physical examination showed a normal pulse rate and blood pressure. On auscultation, the first heart sound was normal. Laryngoscopy revealed a paralyzed left vocal fold. Chest X-ray showed findings suggestive of emphysema. Contrast enhanced chest CT image showed a dissection-like giant aneurysm in the aortic arch directed inferiorly. Cardiomegaly did not appear (Fig. 4A–C). ECG showed atrial flutter with variable atrioventricular (AV) block and left ventricular hypertrophy with QRS widening. The patient underwent TEVAR at our hospital (Fig. 4D). Echocardiography showed mild atrial regurgitation with dilated sinus portion of the ascending aorta (40 mm) and good flow through TEVAR stent graft. Injection laryngoplasty was performed after TEVAR. We injected 0.5 cc of hyaluronic acid into the mid portion of the membranous vocal fold (Fig. 2C, F). His voice was immediately improved after the initial injection. We are currently following him up and we plan to perform repeat injection when his voice is aggravated. The initial GRBAS score was 7 and final GRBAS score was 3.
Discussion
The causes of RLN paralysis have been mainly classified as idiopathic, surgical trauma, and cancer invasion of the thyroid, lung and esophagus. However, RLN paralysis very rarely occurs secondary to compression caused by anomalies of the heart or great vessels. Norbert Ortner, an Austrian physician, reported left RLN paralysis in a patient with mitral valve disease.1) After that, various cardiac disorders causing RLN paralysis have been suggested such as left ventricular failure, atrial septal defect, patent ductus arteriosus (PDA), primary pulmonary hypertension, recurrent pulmonary artery embolism, mitral regurgitation, atrial myxoma, left ventricular aneurysm, cor pulmonale, and various types of aortic aneurysms.3–8)
In the normal course of RLNs, the left RLN comes from the left vagus nerve near the aortic arch’s anterolateral border, in the area between the main pulmonary artery and the aortic arch. It is located just behind the ligamentum arteriosum and it ascends in the groove between the trachea and the esophagus. The right RLN travels between the trachea and the esophagus by crossing the initial segment of the subclavian artery and hooking around it. Result, a dilated pulmonary artery, a persistent ductus arteriosus, or an aortic arch aneurysm may cause nerve compression.6–8) Fetterolf et al. reported that in Ortner’s syndrome, because the aorta and the pulmonary artery are just 4 mm apart in the aorto-pulmonary window, the nerve is compressed between the aorta, ligamentum arteriosum, and the left pulmonary artery.7) Other possible theories reported include lymphadenitis and scarring in the aortic window causing nerve fixation, pressure from the left bronchus, right ventricular hypertrophy, pulmonary artery atherosclerosis, anatomical position of the ligamentum arteriosum or a dilated pulmonary artery.5,6) Some patients with arteriosclerotic heart diseases suddenly suffer left RLN paralysis because rapid onset of left ventricular failure produces sudden pulmonary hypertension with acute pulmonary vessel dilatation. This phenomenon is known as dynamic dilatation. Hoarseness associated with abrupt cardiac aggravation has been recorded in patients with long-standing PDA, lending credence to the above assertion.11,12) The degree of recovery from voice change after endoluminal treatment of aneurysm was variable.13,14) Morales et al. reported among 8 patients with Ortner’s syndrome which had endovascular repair of the aneurysm, voice of 3 patient had improved within a mean of 24 months follow-up.15)
Injection laryngoplasty is a surgical procedure used to treat glottal insufficiency in patients with unilateral VFP. Glottal insufficiency is a condition whereby patients suffer from weak and breathy voice due to air escape through incompletely opposed vocal folds. The aim of injection laryngoplasty is to move the paralyzed vocal fold medially to aid voice production by opposing the gap. Injection laryngoplasty has evolved in terms of its approaches and materials.16,17) However, there is no ideal injection material. The ideal injection material should be biocompatible, inert and should not cause a local tissue reaction or fibrosis. The injection substance should be easily accessible, easy to measure in quantity, and simple to inject using a little needle. Also, it should maintain the viscoelasticity of the vocal folds after injection.18) Hyaluronic acid is a natural polysaccharide which is part of the extracellular matrix, found in the lamina propria of vocal folds. Rheologic studies have shown that injection materials based on hyaluronic acid have viscoelastic characteristics that are most similar to human vocal folds. It has low tissue reactivity, and therefore, it has a good safety profile. Hyaluronic acid-based injection materials generally last for about 4–6 months. However, some studies have shown that they can last up to 12 months. There is also a possibility of an allergic reaction towards the injection material.19) It is important to evaluate the patients’ allergy history and to ensure that the resuscitation trolley is readily available in the event of an emergency. There is a possibility of patients showing a less than satisfactory outcome. This can be attributed to migration or increased rate of resorption of the injection material. Rarely, it could be due to accidental injection at the wrong site, thereby providing no effect on the patient’s voice. In some instances, the materials can be wrongly injected into the vocal cords, causing edema and therefore, hoarse voice, discomfort or even breathing difficulty. The risk of bleeding from injection is low.20,21) The cricothyroid approach is the most common method. This approach has some disadvantages: the anatomical landmark may not always be readily identifiable especially in obese patients and in patients with previous neck surgery. In addition, because of the oblique direction of injection, determining the depth and placement of the needle tip can be challenging at times.
In conclusion, Ortner’s syndrome also known as cardiovocal syndrome is an uncommon condition that can be caused by a variety of cardiopulmonary disorders. The mechanism of Ortner’s syndrome is thought to be compression of the RLN by an abnormal cardiovascular structure. Therefore, we should routinely perform laryngoscopic examination in all cases of heart disease presenting with hoarseness of voice. Injection laryngoplasty is a useful and simple procedure as a means of treating VFP secondary to cardiovascular disease.






