Introduction
Mucormycosis of the nasal cavity and paranasal sinuses is a rare but opportunistic infection of the class Phycomycetes, order Mucorales. It is highly aggressive and causes a rapidly progressive, life-threatening disease, especially in patients with diabetes or immunosuppressed patients. The most effective treatment consists of immediate surgical debridement, administration of systemic antifungal drugs, recovery of compromised immunity.1,2) However, asymptomatic or chronic indolent type of mucormycosis can be observed in immunocompetent patients.1–3) There is no consensus of treatment for indolent sinonasal mucormycosis patients.
In this study, we collected 9 cases of mucor fungal balls and assessed the clinical and radiologic results of indolent mucormycosis of paranasal sinus in healthy patients treated by endoscopic sinus surgery (ESS) alone.
Materials and Methods
A retrospective review of nine patients with the diagnosis of chronic indolent mucormycosis of paranasal sinus and treated by ESS alone between 2007 and 2017 was performed. Institutional Review Board approval was obtained from the (IRB number 2018-0153). Informed patient consents were waived because it was a retrospective chart review. The following data were collected from the medical records: age, gender, clinical presentations, pre- and post ESS endoscopic findings, underyling diseases, histopathology, pre- and postoperative radiologic findings.
Radiologic images were reviewed to assess the involved side and sinus, changes of bony sinus wall.
Results
Nine patients were identified as having a diagnosis of indolent paranasal sinus mucormycosis. They consists of 2 men and 7 women. The mean age was 65.7 (range, 48–77 years). Our patients have nasal symptoms included facial pain, nasal stuffiness, postnasal drip and foul odour. All patiens had previously healthy and reported no underlying disease, medication, facial trauma with the exception of four patients with well controlled two hypertension patients and two diabetes patients (Table 1).
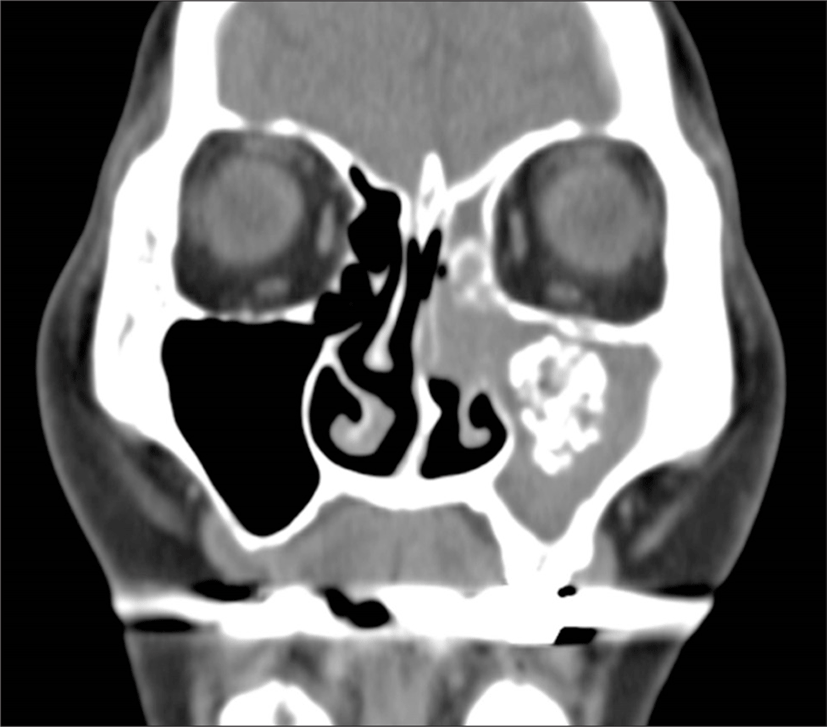
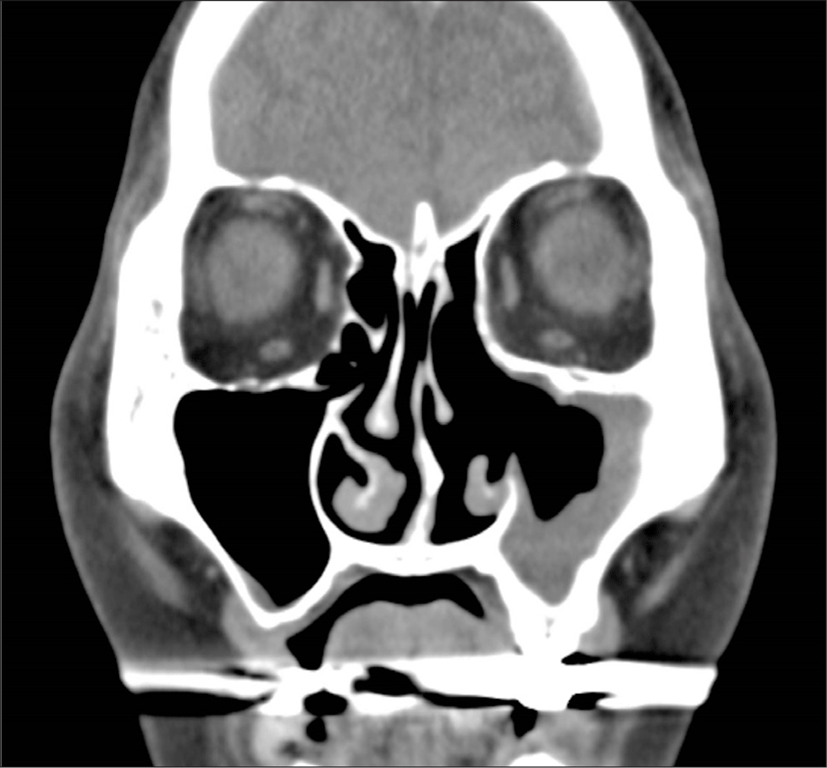
Preoperative paransal sinus computed tomography (CT) showed total or partial opacification of the unilateral maxillary sinus with focal calcifications without bony destruction of the involved sinus or invasion of the orbit or brain in all patients (Fig. 1). Five patients had inflammatory nasal polyps in the involved paranasal sinus (Fig. 2).
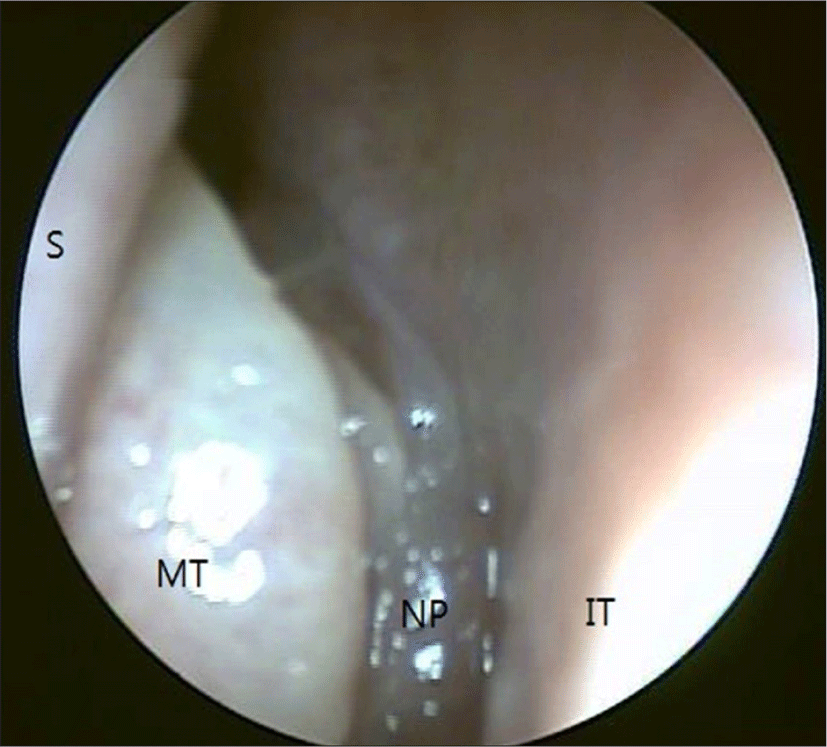
All patients underwent ESS based on clinical symptoms, paranasal CT with suspicision of fungal sinusitis. Surgical procedures included uncinectomy, ethmoidectomy and middle meatal antrostomy with removal of clay like, thick brownish- green material. After surgery, the patients were given antibiotics for 3 days and then discharged for general protocol for fungal ball.
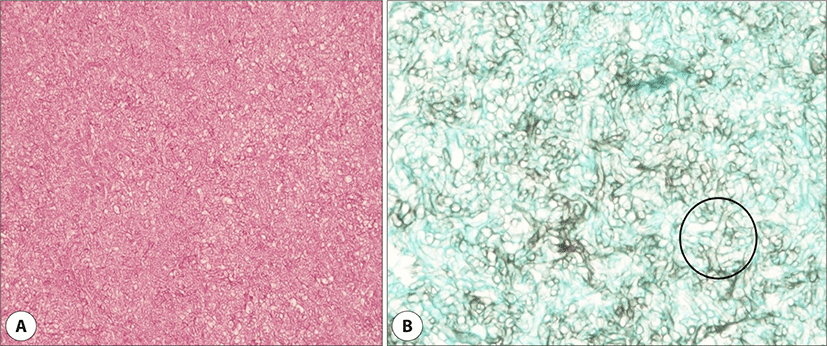
The histopathologic findings showed mucormycosis with broad, non-septated, right-angled hyphae (Fig. 3). In spite of diagnosis of mucormycosis, the patients were not any antifungal agents after surgery.
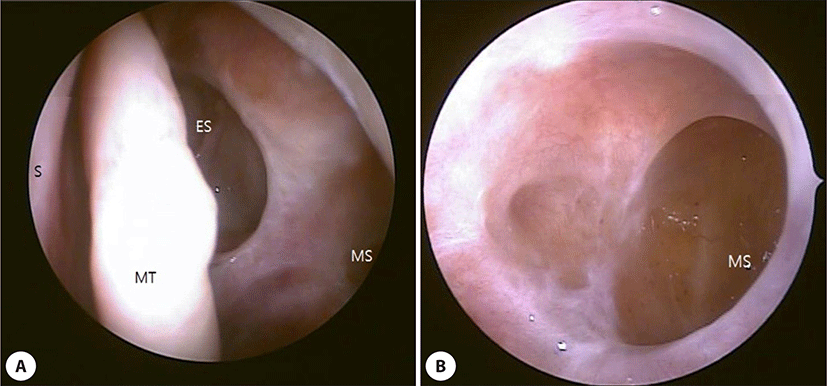
All patients had monthly angled endoscopic follow up (Fig. 4) and postoperative 3 months paranasal CT follow up (Fig. 5). The average follow up duration was 11.7 months. There was no recurrence.
Discussion
Mucormycosis is a clinical disease caused by fungi from 4 families of the Mucorales, which is a member of the class Zygomycets. The zygomycetes are hyaline fungi commonly found in breads and fruits. They are ubiquitous in soil, in vegetation, and in the air, making them frequent inhabitants of the upper airway mucosa but do not become an infectious source in healthy people.1,4) They become pathogenic when the patient’s resistance has been changed.4)
Some studies suggest that mucormycosis is an opportunistic infection in approximately 5% to 12% of all fungal infections in the high-isk group.5)
Rhinocerebral or craniofacial zygomycosis is a common form and usually fatal or fatal. Typically, the patient is at high risk for leukopenia or metabolic acidosis. Diabetes mellitus is the single most common disease associated with the development of invasive mucormycosis.5,6) In this study, two patients were presented with diabetes mellitus, but all were well-controlled, and did not show any signs of acidosis and appeared to be non- invasive fungal ball.
Rhinocerebral mucormycosis is the most common form, accounting for one-third to one-half of all mucormycosis.5) The first symptom of rhinocerebral murcomycosis is sinusitis or periorbital cellulitis,7,8) followed by suffusion of conjunctiva, blurry vision, and soft tissue swelling after ocular pain, facial pain, facial numbness.9,10) If not treated, the infection spreads from the ethmoid sinus to the orbit, resulting in extraocular muscle dysfunction and proptosis. Severe chemosis may also be seen. Involvement of the controlateral eye is an ominous finding suggesting cavernous sinus thrombosis when bilateral proptosis, chemosis, vision loss, and ophthalmoplegia occur.5) Progressive vision loss may be due to optic nerve involvement or infarction10–13) or cavernous sinus thrombosis. Upon naso-endoscopic examination, mucosal findings may appear normal at the very early stages of fungal spread. If the infected tissue then progress through an erythematous phase, ultimately forms black, necrotic eschar as the thrombosed blood vessels and tissue infarction occurs.14,15)
However, indolent rhinocerebral mucormycosis in immunocompetent patients is often characterized by subtle symptoms and signs.16,17) The symptoms in this study were facial pain, nasal stuffiness, foul odor, postnasal drip and non - specific features and similar pattern to chronic sinusitis and fungal ball. No necrotic eschar was observed in the endoscopic findings.
The treatment of invasive mucormycosis requires reversal of the predisposing factors, aggressive surgical removal of infected tissue and systemic antifungal medical therapy.5,16)
There is no consensus on the extent of surgery in the treatment of mucormycosis. Endoscopic surgery is best suitable for earlier and limited disease. In particular, there is uncertainty about the appropriate treatment of limited sinonasal mucormycosis in obvious healthy subjects. These patients are more benign and tend to be localized. Some reports showed that limited mucormycosis can be cured with surgical debridement alone2,18) or with combination of surgery following a course of amphotericin B.16) In previous study, authors reported that indolent mucormycosis of paranasal sinus in four case series immunocompetent patients could be treated by endoscopid sinus surgery alone, and antifungal drugs may not be needed.2) In this study, we showed that, in nine case series, paranasal indolent mucormycosis of healthy patient could be treated by ESS alone.
Conclusion
Paranasal sinus mucormycosis is very rare in healthy patients. This study still includes a small number of patients. However, ESS alone is thought to be sufficient for the treatment of chronic indolent cases in immunocompetent patients without evidence of invasion and antifungal treatment may not be necessary.






